Here's how over-the-counter birth control could disrupt limited access to contraception
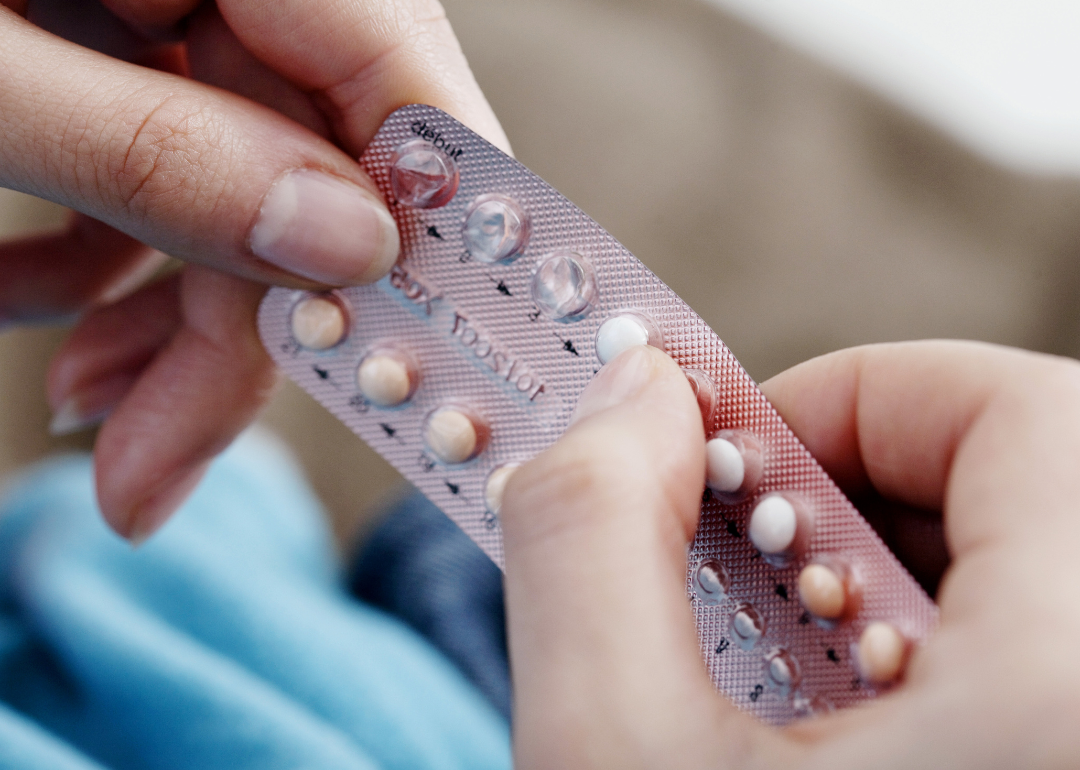
Image Point Fr // Shutterstock
Here’s how over-the-counter birth control could disrupt limited access to contraception
Close-up of hands holding oral contraceptive pills.
On June 24, 2022, the Supreme Court issued its decision on Dobbs v. Jackson Women’s Health Organization, effectively overturning the abortion protections provided in the court’s previous decision on Roe v. Wade. Since that decision, the status of contraceptive and abortion access across the country has been in question, with some states moving to protect access while others attempt to strip it away.
Because abortion access is no longer considered a universal right under federal law, access to varied and comprehensive contraception has become more important than ever. Contraception is any method used to prevent a pregnancy from happening in the first place. This includes a range of methods such as hormone pills, IUDs, and even condoms. In contrast, abortions are procedures that end an existing pregnancy and can include the use of either pill-based medication or an in-clinic procedure.
In May 2023, a scientific advisory board to the Food and Drug Administration voted to recommend that the agency approve a hormone-based birth control pill called Opill for over-the-counter use. Opill contains a synthetic replica of the hormone progesterone in order to help prevent pregnancy. While Opill utilizes only one hormone, most other birth control pills on the market today also contain some amount of estrogen. All 17 board members voted in favor of approval, voicing the positive impact increased access to contraception would have nationwide in the wake of the Dobbs decision.
As the FDA weighs the advisory board’s recommendation, Stacker investigated how access to contraception currently varies across the U.S. and how the potential approval of OTC birth control could expand access nationwide using a range of news sources along with an exclusive interview with Tara Mancini, director of public policy at Power to Decide.
![]()

BongkarnGraphic // Shutterstock
Current access to contraception is uneven across the country
Doctor and patient consultation.
According to Power to Decide’s contraceptive deserts map, vast swaths of communities in the U.S. have little to no access to health centers that offer the full range of contraceptive methods, which include intrauterine devices, birth control pills, implants, the ring, the patch, the shot, diaphragms, cervical caps, and emergency contraception. There is a particularly significant dearth of access through the Midwest, stretching from North Dakota down to Texas.
Very few states have consistent contraceptive access statewide. For instance, people living in the northern areas of Michigan have generally good access to contraceptive methods, with the majority of counties falling into the top two categories with the most access. On the other hand, people living in Michigan’s southern counties are far more likely to have limited access, with many being at the other end of the spectrum with the least access. Utah serves as another example of this divide but with a split between the eastern and western portions of the state.
Speaking with Stacker, Tara Mancini said that in the discussions the FDA scientific advisory board had before recommending that the agency approve Opill for OTC use, “we heard from lots of folks speaking about what the benefits would be for communities, including young people, communities of color, communities with low incomes, and migrant communities.”
Beyond just approving Opill for OTC use, Mancini mentioned the importance of not putting too many restrictions on the medication or pricing it out of range for low-income individuals. In particular, they emphasized ensuring that accessing Opill does not have an age requirement because this could prevent young people and people without official identification, who are often at-risk groups for unplanned pregnancies, from using this form of contraception.

i viewfinder // Shutterstock
Battles for access are primarily happening at the state and local level
Pharmacist holding medication box.
“In 2021, Missouri legislators tried to carve out coverage for emergency contraception and IUDs from Medicaid coverage in one of their must-pass Medicaid bills,” Mancini told Stacker. “It ended up not passing with that exclusion, but this is something that advocates have said has been brought up before, so we expect to see other efforts like that.”
More recently, the Dent County Health Center in Salem, Missouri, called an emergency meeting because one member of the board saw a post on Facebook that mentioned that the local health department had been providing free emergency contraception. The board member believed that post-sex emergency contraception could cause an abortion, which is false.
“Whether this person is misinformed or purposely trying to promote the idea [that contraception is the same as abortion], we have seen misinformation and disinformation around birth control even before Roe, especially with methods like emergency contraception, which many people, even sometimes physicians, have confused with the abortion pill, which it is not. It cannot disrupt a pregnancy, it can only prevent a pregnancy from occurring in the first place,” explained Mancini.
This misinformation can be particularly potent when it comes from leaders and members of communities who have built trusting relationships with people seeking guidance and information. As a result, whether a community generally supports the availability of a variety of contraceptive methods can hinge on the actions and decisions of local and state authorities because they have more direct influence. By the same token, it is up to individual pharmacies to properly provide Opill in stores should it be approved for OTC use in the same manner it is currently up to them to properly provide emergency contraception, colloquially known as Plan B.
“Since emergency contraception came over the counter, there have been lots of surveys of pharmacies and how they handle it,” Mancini explained. “There’ve been numerous secret shopper surveys where folks have gone into a pharmacy and had to ask for it [as though] someone kept it behind the counter. We did one in our office locally, and there weren’t any over-the-counter. The person went and asked the pharmacist about it, and they said, ‘Oh yeah, I always hide some over here for people,’ and it was behind the photo counter or something.”
Mancini said that this can pose a significant barrier to people trying to access this type of medication at a micro-level, especially if a person feels nervous asking for help.
areeya_ann // Shutterstock
Federal actions can have significant impact
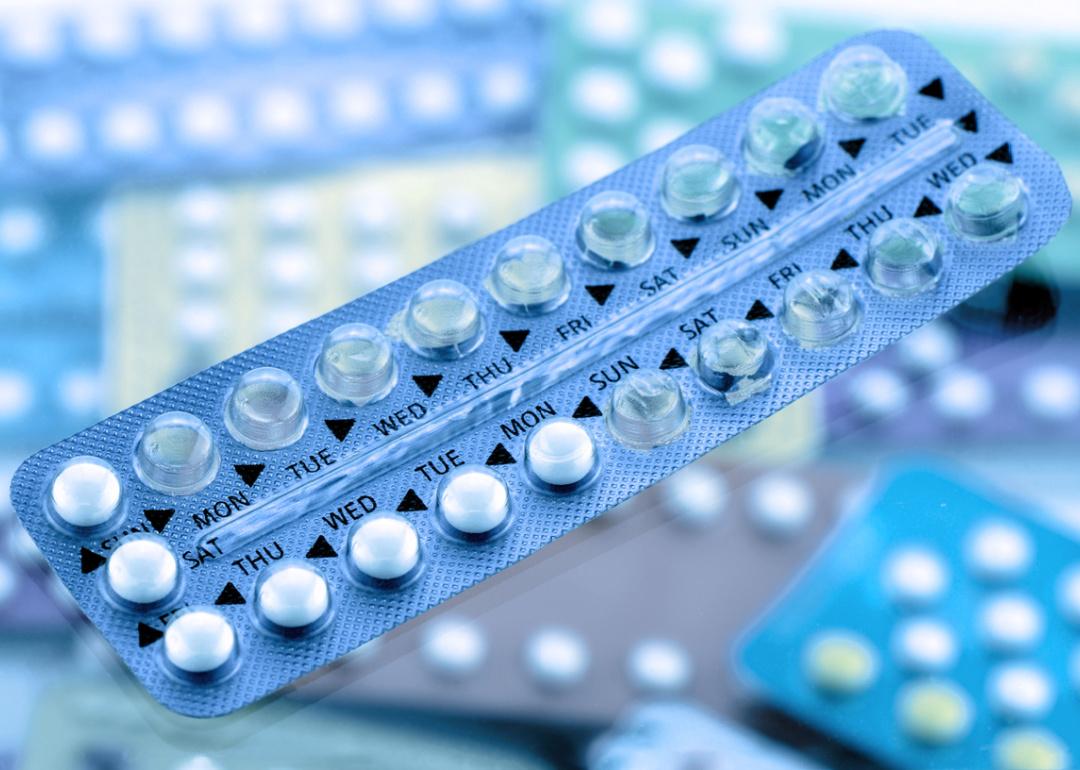
Oral contraceptive pill packages.
Similar to how one Supreme Court decision had a cascading impact where nearly half of all states now restrict abortion rights in some capacity, federal actions with respect to contraceptive access are equally important. Roe v. Wade was originally decided on the principle of privacy implied in the 14th Amendment. A similar justification was used in the case of Griswold v. Connecticut, which protects the right to contraception. Though Mancini said there is some concern that Griswold will meet the same fate as Roe, they were also quick to point out there are other federal resources and regulations of contraception beyond Supreme Court decisions.
“The Title X family planning program, Title X of the Public Health Service Act, provides the only safety net funding for birth control and STI testing in the country and it has been basically flat-funded for almost a decade, despite a rise in costs and rise in need,” Mancini said. “It’s been flat-funded at $286.5 million. Experts have found that the program would need at least $737 million a year to actually keep up with demand, so it is way underfunded at the moment, but it is a pivotal, critical piece of funding that goes to clinics and communities around the country.”
Mancini explained that a wide variety of organizations can draw from this funding, from local health departments to Planned Parenthood clinics, depending on how the particular state allocates it. They noted that because of associated regulations, the funding affords clinics the ability to provide comprehensive reproductive care that is tailored to the community’s culture and individual needs. The approval of Opill for OTC use could make it easier for clinics like those funded by Title X to provide a daily pill as one of a range of contraceptive methods to those who come to them for guidance.

Ground Picture // Shutterstock
Conversations about access to contraception will continue for years
Pharmacist discussing medication with customer.
Due to the splintered nature of discussions about contraception, Mancini believes that the end to the fight for contraceptive access is nowhere in sight, even if the FDA approves Opill for OTC use.
“Opill will be right for some people who don’t have access to a clinic or can’t afford it, but it won’t be right for everybody. So it’s not going to be a panacea for the problem of contraceptive deserts,” they said.
Just as providing a range of options for treating any ailment allows people to choose the right path for them, making a variety of contraceptive options readily accessible can help the greatest number of people plan their families effectively. Each of those options will be considered, researched, and weighed as America continues its political wrestling match over the right of all people to control what they do with their own bodies.
“There’s rarely ever a silver-bullet policy solution,” said Mancini. “[Opill] is one piece of a puzzle.”
Story editing by Brian Budzynski. Copy editing by Tim Bruns.



